This content was originally published by the Longmont Observer and is licensed under a Creative Commons license.
Eric Galatas - Colorado News Connection
DENVER -- Colorado lawmakers are considering a bill that would expand access to telemedicine through Colorado's community health centers, which provide care for 27% of the state's Medicaid clients.
Currently centers are not reimbursed by Medicaid for remote visits, but HB 20-1092 would affirm that telemedicine services meet the definition of a face-to-face visit. Polly Anderson, vice president for strategy and financing with the Colorado Community Health Network, said remote visits are sometimes a patient's best option - especially during flu season.
"When you're sick and you might be contagious, to the extent that some of that can be diagnosed through symptom description or what your temperature is, it keeps that sick person out of the waiting room," Anderson said. "They're not waiting there next to a child maybe that's there for a well-baby visit."
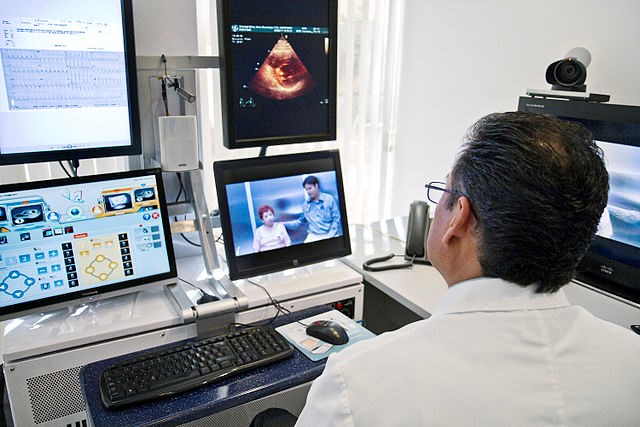
Telemedicine cuts travel and wait times dramatically. Patients need only pick up their smartphone or sit down at a computer at their appointed time.
The measure is set to be heard by the Public Health Care and Human Services committee on Wednesday. An estimate of any additional costs the bill might add to the state's Medicaid tab has not yet been issued.
Anderson said telemedicine is especially convenient for people with chronic conditions such as diabetes and high blood pressure, where a doctor-patient relationship already is established.
The state's homeless population also stands to benefit. Social workers can connect clients with medical care from anyplace with cell service. Anderson said she believes the measure will reduce Colorado's overall Medicaid expenses because more people will be able to access primary care.
"Primary care is a key component in preventing and treating illnesses before they get worse - before they would result in an emergency room visit, or worse, in a hospital admission," she said.
The measure also would allow the costs of clinical pharmacists - a key part of a health center's team-based approach - to be included in reports submitted to Medicaid for reimbursement. Clinical pharmacists help ensure patients get the best medicine available, at the best price, and with less chance of negative interactions between medications.

.jpg;w=120;h=80;mode=crop)
